Overview
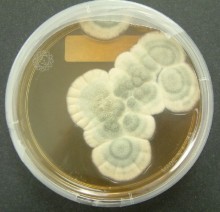
Penicillin refers to a family of antibiotics that share a beta-lactam core and are active against many types of bacteria. First observed as a natural compound produced by molds of the genus Penicillium, penicillins are bactericidal agents widely used to treat infections caused by susceptible organisms. They remain important in clinical medicine because of their targeted activity against Gram-positive cocci and other bacteria, their relative safety for many patients, and their affordability in many settings.
Chemical nature and mechanism
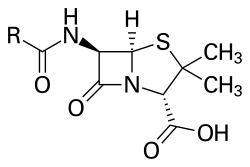
All penicillins contain a characteristic four-membered beta-lactam ring fused to a thiazolidine ring. This structure binds to bacterial penicillin-binding proteins (PBPs), enzymes involved in the final stages of cell wall biosynthesis, and thereby inhibits peptidoglycan crosslinking. The result is weakening of the cell wall and bacterial cell lysis. Medicinal chemists have modified the side chains attached to the core scaffold to produce derivatives with different spectra of activity, stability to stomach acid, or resistance to bacterial beta-lactamases.
History of discovery and development
Penicillin was first noticed in 1928 when Alexander Fleming observed that a contaminating mold inhibited bacterial growth on a culture plate. The active substance was later developed into a practical therapeutic agent in the late 1930s and early 1940s through the work of researchers who devised methods for purification and mass production. The initial availability of penicillin transformed treatment of bacterial infections and reduced deaths from wound infections and pneumonia during and after World War II. For their roles in its discovery and development, Fleming and later researchers received wide international recognition.
Clinical uses and important examples
Different penicillins are used for different infections. Natural penicillins (such as benzylpenicillin and phenoxymethylpenicillin) are effective against many streptococci and some pneumococci, and remain choices for conditions such as streptococcal pharyngitis, certain forms of meningitis, and syphilis. Aminopenicillins and other semisynthetic derivatives extend activity to additional Gram-negative organisms or offer improved oral bioavailability. Clinicians select a specific agent based on the infecting organism, site of infection, and patient factors.
Resistance, limitations and modern responses
Bacterial resistance to penicillins is widespread and arises chiefly by production of beta-lactamase enzymes that hydrolyze the beta-lactam ring, by mutations in PBPs that reduce drug binding, or by reduced drug access to targets. To counter resistance, scientists developed beta-lactamase–stable penicillins, beta-lactamase inhibitors used in combination therapies, and entirely different antibiotic classes. Ongoing surveillance and stewardship programs aim to preserve effectiveness by encouraging appropriate use.
Safety and allergies
Penicillins are generally well tolerated, but allergic reactions are the most clinically important adverse effect. Reactions range from minor rashes and gastrointestinal symptoms to severe, potentially life-threatening anaphylaxis in a small proportion of patients. A reported penicillin allergy in a patient's history should prompt careful assessment; many people labeled “penicillin-allergic” are not truly allergic when formally tested, and alternative therapies may be less effective or more toxic.
Further reading and related topics
- Bacterial infections and penicillin
- Staphylococci: characteristics and treatment
- Streptococci and susceptibility to penicillins
- Antibiotic resistance overview
- Alexander Fleming biography
- Fleming's original observations
- The genus Penicillium and natural products
- Treatment of syphilis with penicillin
- Tonsillitis and antibiotic choices
- Meningitis management
- Pneumonia and antimicrobial therapy
- Penicillin use in wartime medicine
- Fleming's petri dish observation
- Howard Florey and early development
- Florey's contributions to mass production
- Ernst Boris Chain and purification work
- Nobel Prize awarded for penicillin work
- Penicillin allergy: recognition and testing
- Common symptoms of drug allergy
- Gastrointestinal side effects
- Diarrhea associated with antibiotics
- Fever as an adverse reaction
- Nausea and vomiting with antibiotics
- Serious skin reactions and drug safety
For clinical decisions, consult current treatment guidelines and infectious disease specialists. Historical summaries and scientific principles described here are general; specific dosing, interactions, and resistance patterns vary by region and over time.